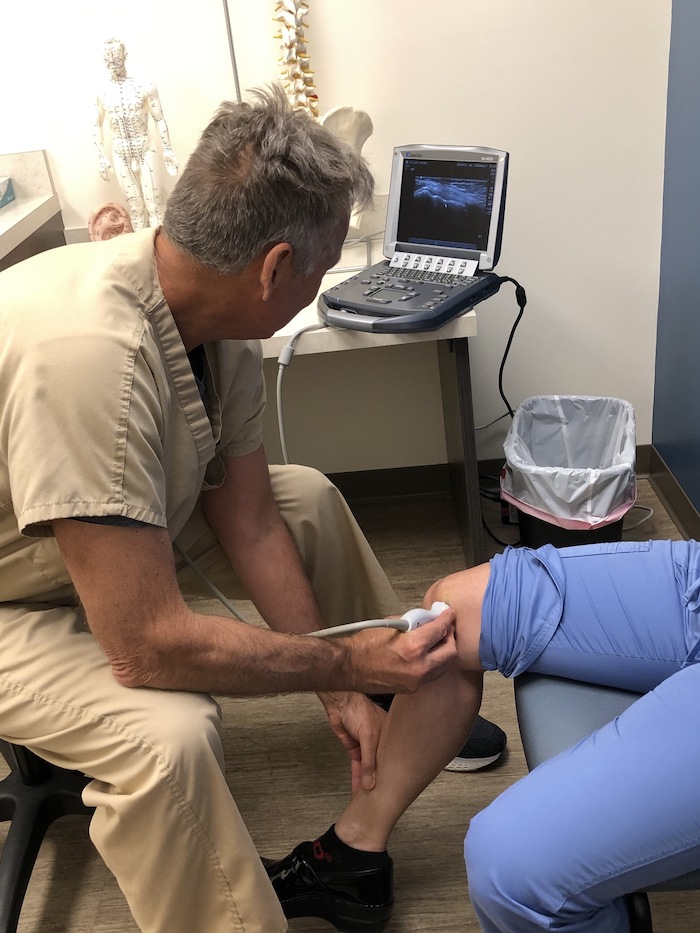
Multipotent adult mesenchymal stem cells are extensively investigated - in particular their behaviour in cell culture: how do they stay multipotent after several passages how is chondrogenesis triggered in MSCs. MSCs were first identified in the pioneering studies of Friedenstein and Petrakova (1966) and are of major interest of research in the treatment of arthritis, in particular OA. Regardless of their origin they have the capacity to differentiate into many cell types, including cells of connective tissue lineages, including bone, fat, cartilage and muscle. MSCs can be harvested from bone marrow, periosteum, trabecular bone, adipose tissue, synovium, skeletal muscle and deciduous teeth. Pittenger et al have described that MSCs could be cultured without losing their multilineage differentiation potential and it has been shown that MSCs are capable of undergoing chondrogenic differentiation both in-vitro and in-vivo. The stem cell candidates for use in these therapies are multipotent adult MSCs, because they are available in several tissues, including in the fluid inside the joint, and have the ability to differentiate into cells of the chondrogenic lineage. 
However, osteoarthritis cannot be cured by any radical treatment at the moment. This treatment should be used in conjunction with additional treatment in order to improve patients’ functional status and quality of life. The aim in using stem cells is to support the self-healing process of the knee joint cartilage which results in relief from OA symptoms. Construction workers, especially floorers, also have a significantly elevated prevalence of knee OA. Additionally, ross-sectional studies indicate that the risk of knee OA is 1.9 to 13.0 times higher among underground coal miners when compared to a control population presumably, due to frequent work in the kneeling or squatting position. Recently, a number of genome wide association studies (GWAS) ( e.g., Rotterdam GWAS, Tokyo GWAS, Chingford Study) have highlighted the significance of gene mutations ( e.g., in GDF5) for the development of knee OA. A variety of endogenous ( e.g., age, sex) and exogenous (obesity, patient’s lifestyle) risk factors for OA have also been outlined. In regards to the epidemiology of knee OA (Table (Table1), 1), studies indicate that knee osteoarthritis in men aged 60 to 64 is usually found in the right knee (23%) than in the left knee (16.3%), while distribution seems to be more evenly balanced in women of the same age (right knee, 24.2% left knee, 24.7%). It is believed that synovial inflammation is a response of synovial macrophages to cartilage debris and catabolic mediators entering the synovial cavity. Moreover, it correlates to clinical signs of knee OA such as swelling of the knee and inflammatory pain. Recently, synovial inflammation has also been accredited as a factor limiting knee cartilage repair. The pathogenesis of knee OA have been linked to biomechanical and biochemical changes in the cartilage of the knee joint ( e.g., inability to withstand normal mechanical stresses, limited supply of nutrients and oxygen, inadequate synthesis of extracellular matrix components, increased synthesis of tissue-destructive proteinases (matrix metalloproteinases and aggrecanases) and overall apoptosis of chondrocytes). Comparison between a normal and diseased joint (Illustration created after Felson and Buja et al) Furthermore, based on their critical assessment of the present academic literature the authors of this review share their vision about the future of stem cell applications in the treatment of knee osteoarthritis. In addition to the latest advances in the field, challenges associated with stem cell therapy regarding knee cartilage regeneration and chondrogenesis in vitro and in vivo are also outlined and analyzed. 
The aim of this review is to outline the latest advances in stem cell therapy for knee osteoarthritis as well as highlight some of the advantages of stem cell therapy over traditional approaches aimed at restoration of cartilage function in the knee. Total knee replacements come together with high effort and costs and are not always successful. Moreover, in severe cases of knee osteoarthritis total knee replacement may be required. While conventional treatments like physiotherapy or drugs offer temporary relief of clinical symptoms, restoration of normal cartilage function has been difficult to achieve. By some estimations in 2030, only in the United States, this medical condition will burden 67 million people. It is characterized by degeneration of the cartilage substance inside the knee which leads to pain, stiffness and tenderness. Knee osteoarthritis is a chronic, indolent disease that will affect an ever increasing number of patients, especially the elderly and the obese.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
